
When should your teen or tween start using skin products?

Social media and stores are full of products that promise perfect skin. Increasingly, these products are being marketed not just to adults but to teens and tweens. Many are benign, but some can cause skin irritation — and can be costly. And even if these products are benign, does buying them support unhealthy notions about appearance and beauty?
It’s worth looking at this from a medical perspective. Spoiler alert: for the most part teens and tweens do not need specialized skin products, especially expensive ones. But let’s talk about when they may make sense.
When can a specialized skin product help tweens and teens?
So, when should your child buy specialized skin products?
- When their doctor recommends it. If your child has a skin condition that is being treated by a doctor, such as eczema or psoriasis, over-the-counter skin products may help. For example, with eczema we generally recommend fragrance-free cleansers and moisturizers. Always ask your doctor which brands to choose, and get their advice on how best to use them.
- If they have dry and/or sensitive skin. Again, fragrance-free cleansers are a good idea (look for ones recommended for people with eczema). So are fragrance-free, non-irritating moisturizers (look for creams and ointments rather than lotions, as they will be more effective for dry skin). If you have questions, or if the products you are buying aren’t helping, check in with your doctor.
What about skin products for acne?
It’s pretty rare to go through adolescence without a pimple. Many teens aren’t bothered by them, but if your child is bothered by their pimples or has a lot of them, it may be helpful to buy some acne products at your local pharmacy.
- Mild cleansers tend to be better than cleansers containing alcohol. You may want to check out cleansers intended for dry skin or eczema.
- Over-the-counter acne treatments usually contain benzoyl peroxide, salicylic acid, azelaic acid, or alpha-hydroxy acids. Adapalene can be helpful for more stubborn pimples.
- Steer away from astringents or exfoliants, which tend to irritate the skin.
- Talk to your doctor about what makes the most sense for your child — and definitely talk to them if over-the-counter products aren’t helpful. There are many acne treatments available by prescription.
Ask questions and help dispel myths
If your teen or tween doesn’t fall into one of these groups, chances are they don’t need anything but plain old soap and water and the occasional moisturizer if their skin gets dry.
If your child has normal, healthy skin yet is asking for or buying specialized skin products, ask them why. Do your best to dispel the inevitable marketing myths — like that the products will prevent problems they do not have. Let them know that should a problem arise, you will work with them — with the advice of their doctor — to find and buy the best products.
Use it as an opportunity, too, to talk about self-image and how it can be influenced by outside factors. This is an important conversation to have whether or not your child is pining for the latest cleanser they see on Instagram. Helping your child see their own beauty and strengths is a key part of parenting, especially for a generation raised on social media.
About the Author

Claire McCarthy, MD, Senior Faculty Editor, Harvard Health Publishing
Claire McCarthy, MD, is a primary care pediatrician at Boston Children’s Hospital, and an assistant professor of pediatrics at Harvard Medical School. In addition to being a senior faculty editor for Harvard Health Publishing, Dr. McCarthy … See Full Bio View all posts by Claire McCarthy, MD

Co-regulation: Helping children and teens navigate big emotions

When preschoolers are melting down or teens are slamming doors, parents face two difficult tasks: keeping themselves composed and supporting their kids’ ability to self-soothe while building skills to handle future challenges.
These abilities are at the heart of co-regulation, a parenting tool that requires patience and practice. But what exactly is involved, and how does it help support children and teens wrestling with big emotions?
What is co-regulation?
“Co-regulation is a supportive, interactive, and dynamic process,” says Lauren Marchette, a child, adolescent, and family psychologist and a lecturer in psychiatry at Harvard Medical School.
Through warm and responsive interactions, caregivers help young people learn better ways to regulate their emotions during the inevitable upsets and challenges of life. “At its heart, co-regulation is connecting with a child who’s in distress and being able to evaluate what that child needs in the moment to help calm themselves.”
But before a parent or trusted adult can help a child, they need to understand — and possibly expand — their own emotional skills and limitations. Emotions are often contagious, whether a person is upset or sharing a sense of calm.
“The tricky part of co-regulation is that adults have to recognize how they’re feeling and be able to regulate their own emotions in difficult moments so they can help children to gain these same skills,” Marchette says. “But this will be so important for kids to develop healthy relationships over time, and affects how people do in school, work, and life in general.”
How does building emotional skills help children and teens?
As children grow up, they learn different skills — how to build a block tower, play a sport, or solve a math equation. They also learn emotional skills: how to recognize and handle feelings of anger or anxiety, for example.
Known as self-regulation, such emotional skills are truly the basis of wellness in life, Marchette says. By consistently practicing co-regulation, parents and other trusted adults foster self-regulation skills in kids.
The list of self-regulation skills is wide-ranging, involving
- emotional awareness and literacy, including the ability to identify emotions
- emotional regulation skills such as self-soothing
- perspective-taking, or the ability to "walk in another’s shoes”
- social skills such as taking turns and practicing patience
- paying attention and remaining focused when needed
- problem-solving
- thinking flexibly
- time management skills
- goal-setting.
What are the potential benefits of co-regulation?
Co-regulation enables kids to eventually learn to
- handle stress
- resist immediate gratification
- avoid hasty, ill-informed decisions
- make and stick to plans
- solve problems
- adapt to challenges
- take healthy risks.
Some research suggests that having better self-regulation skills is linked to more positive outcomes in life, such as higher income and lower rates of substance use and violence.
Who might especially benefit from co-regulation?
Everyone wins when kids are better able to navigate frustrations and manage their reactions to their thoughts and feelings. Parents, teachers, coaches, guidance counselors, mentors, and other adults who interact closely with children also stand to benefit.
As for kids themselves, it’s hard to think of any whose lives won’t be improved by adults who have invested themselves in practicing co-regulation, Marchette says.
But practicing co-regulation skills with certain children and adolescents — including those whose families are experiencing economic hardship, substance abuse, divorce, or other distressing situations — can be especially important.
Is there evidence that co-regulation works?
“While co-regulation is built upon a solid theoretical framework, not many studies have delved into its effectiveness — at least across all age groups,” Marchette says. “Research that does focuses mainly on infants and preschoolers.”
“Much less is known about how co-regulation interventions work for older youth,” she says. “The research is trying to catch up to what we know from years of clinical experience.”
How can a parent coach a child through co-regulation?
Co-regulation doesn’t stand alone as a skill. It relies on fostering a warm, responsive relationship with children, providing structure, and setting limits. “Children benefit from consistent, predictable routines with clear expectations and consequences,” Marchette says.
When a child begins experiencing big emotions, a co-regulation response will look different depending on the child and circumstances. But the steps to take are similar.
“First, the parent needs to pause and self-regulate their own emotions, such as by taking a deep breath,” Marchette explains. “The next steps are validating the child’s feelings, observing the child’s response, and then deciding how to respond next, including verbally and nonverbally, such as with a touch.”
Marchette offers an example based on her own practice: 12-year-old “Eric” is tackling a writing assignment in his bedroom when his mother suddenly hears loud noises. She walks to his door and finds him throwing a stapler, notebook, and container of pens off his desk. “What’s wrong with me?” he yells. “I suck at writing and I hate school!” Then Eric puts his head down on his desk.
The sixth grader’s mom knows he needs help calming down, so she pauses and takes a deep breath. Then she walks over and whispers his name, placing her hand on his shoulder. After more silence, Eric gradually starts sitting up in his chair. “I can tell how frustrated you are with this assignment,” she says to him, validating his feelings. “It must be a really challenging one.”
Eric’s mother knows he needs a break after he mutters, “I can’t do it.” She suggests a getting a glass of ice-cold water, and Eric glumly follows her to the kitchen. After the break, they can re-evaluate if Eric is ready to return to his homework or needs further coping strategies — like a walk outside or a round of jumping jacks — to get his frustration out.
What resources can help parents practice co-regulation?
The Administration for Children and Families offers a free Co-Regulation in Action video series. And some therapists — especially those who specialize in behavioral parent training or cognitive behavioral therapy — can help parents who feel their skills need a boost.
It’s worth noting that it can be hard to have sufficient resources — emotional, financial, and other supports — to practice co-regulation consistently. Those who wish to try should give themselves some grace as they learn the process. “Even parents who are thinking their own self-regulation skills aren’t where they want them to be should realize this is a muscle they can strengthen,” Marchette says. “It’s important to have that growth mindset.”
About the Author

Maureen Salamon, Executive Editor, Harvard Women's Health Watch
Maureen Salamon is executive editor of Harvard Women’s Health Watch. She began her career as a newspaper reporter and later covered health and medicine for a wide variety of websites, magazines, and hospitals. Her work has … See Full Bio View all posts by Maureen Salamon
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

Ever worry about your gambling?

Are online gambling and sports betting new to your area? Are gambling advertisements catching your eye? Have you noticed sports and news shows covering the spread? Recent changes in laws have made gambling widely accessible, and its popularity has soared.
Occasional bets are rarely an issue. But uncontrolled gambling can lead to financial, psychological, physical, and social consequences, some of which are extreme. Understanding whether gambling is becoming a problem in your life can help you head off the worst of these issues and refocus on having more meaning, happiness, and psychological richness in your life. Gambling screening is a good first step.
Can you screen yourself for problem gambling?
Yes. Screening yourself is easy. The Brief Biosocial Gambling Screen (note: automatic download) is a validated way to screen for gambling disorder. It has three yes-or-no questions. Ask yourself:
- During the past 12 months, have you become restless, irritable, or anxious when trying to stop/cut down on gambling?
- During the past 12 months, have you tried to keep your family or friends from knowing how much you gambled?
- During the past 12 months, did you have such financial trouble as a result of your gambling that you had to get help with living expenses from family, friends, or welfare?
What do your answers mean?
Answering yes to any one of these questions suggests that you are at higher risk for experiencing gambling disorder. Put simply, this is an addiction to gambling. Like other expressions of addiction, for gambling this includes loss of control, craving, and continuing despite bad consequences. Unique to gambling, it also often means chasing your losses.
A yes doesn’t mean that you are definitely experiencing a problem with gambling. But it might be valuable for you to seek a more in-depth assessment of your gambling behavior. To find an organization or person qualified to help, ask a health care provider, your local department of public health, or an advocacy group like the National Council on Problem Gambling.
Are you ready for change?
Your readiness to change a behavior matters when deciding the best first steps for making a change. If someone asks you whether you want to change your gambling, what would you say?
|
I never think about my gambling. |
Sometimes I think about gambling less. |
I have decided to gamble less. |
I am already trying to cut back on my gambling. |
I changed my gambling: I now do not gamble, or gamble less than before. |
Depending on your answer, you might seek out different solutions. What’s most important initially is choosing a solution that feels like the right fit for you.
What if you don’t feel ready to change? If you haven’t thought about your gambling or only occasionally think about changing your gambling, you might explore lower intensity actions. For example, you could
- read more about how gambling could create a problem for you
- listen to stories of those who have lived experience with gambling disorder.
If you are committed to making a change or are already trying to change, you might seek out more engaging resources and strategies to support those decisions, like attending self-help groups or participating in treatment.
Read on for more details on choices you might make.
What options for change are available if you want to continue gambling?
If you want to keep gambling in some way, you might want to stick to lower-risk gambling guidelines:
- gamble no more than 1% of household income
- gamble no more than four days per month
- avoid regularly gambling at more than two types of games, such as playing the lottery and betting on sports.
Other ways to reduce your risk of gambling harm include:
- Plan ahead and set your own personal limits.
- Keep your entertainment budget in mind if you decide to gamble.
- Consider leaving credit cards and debit cards at home and use cash instead.
- Schedule other activities directly after your gambling to create a time limit.
- Limit your use of alcohol and other drugs if you decide to gamble.
What are easy first steps toward reducing or stopping gambling?
If you’re just starting to think about change, consider learning more about gambling, problem gambling, and ways to change from
- blogs, like The BASIS
- books like Change Your Gambling, Change Your Life
- podcasts like After Gambling, All-In, and Fall In, which offer expert interviews, personal recovery stories, and more.
Some YouTube clips demystify gambling, such as how slot machines work, the limits of skill and knowledge in gambling, and how gambling can become an addiction. These sources might help you think about your own gambling in new ways, potentially identifying behaviors that you need to change.
What are some slightly more active steps toward change?
If you’re looking for a slightly more active approach, you can consider engaging in traditional self-help experiences such as helplines and chatlines or Gamblers Anonymous.
Another option is self-help workbooks. Your First Step to Change is a popular workbook that provides information about problem gambling, self-screening exercises for gambling and related conditions like anxiety and depression, and change exercises to get started. A clinical trial of this resource suggested that users were more likely than others to report having recently abstained from gambling.
Watch out for gambling misinformation
As you investigate options, keep in mind that the quality of information available can vary and may even include misinformation. Misinformation is incorrect or misleading information. Research suggests that some common types of gambling misinformation might reinforce harmful beliefs or risky behaviors.
For example, some gambling books, websites, and other resources exaggerate your likelihood of winning, highlight win and loss streaks as important (especially for chance-based games like slots), and suggest ways to change your luck to gain an edge. These misleading ideas can help you to believe you’re more likely to win than you actually are, and set you up for failure.
The bottom line
Taking a simple self-screening test can start you on a journey toward better gambling-related health. Keep in mind that change can take time and won’t necessarily be a straight path.
If you take a step toward change and then a step back, nothing is stopping you from taking a step forward again. Talking with a care provider and getting a comprehensive assessment can help you understand whether formal treatment for gambling is a promising option for you.
About the Author

Debi LaPlante, PhD, Contributor
Dr. Debi LaPlante is director of the division on addiction at the Cambridge Health Alliance, and an associate professor of psychiatry at Harvard Medical School. She joined the division in 2001 and is involved with its … See Full Bio View all posts by Debi LaPlante, PhD
When — and how — should you be screened for colon cancer?

Colon cancer is the second-deadliest form of cancer after lung cancer. If recent messages about colon cancer screening have left you a little confused, that's understandable. In August, the American College of Physicians (ACP) released updated guidance for colon cancer screening that differs from other major organizations, including recommendations from the American Cancer Society (ACS) and the US Preventive Services Task force (USPSTF).
So, what do you need to know?
How does the advice differ?
First, please note that this advice applies only to people at average risk without a family history of colon cancer. If you have family history, or if other health issues put you at higher-than-average risk for colorectal cancer, talk to your doctor about the best course of action for you.
The main point of disagreement relates to the age at which people should start getting screened. The new ACP guidance says 50, while the other two organizations recommend 45. That earlier age is endorsed by the U.S. Multisociety Task Force on Colorectal Cancer. It's also endorsed by many physicians, including Harvard Medical School professor Dr. Andrew T. Chan, a gastroenterologist and director of epidemiology at Massachusetts General Hospital Cancer Center, who helps explain key facts below.
Why do experts suggest starting screening earlier?
"We're facing an unexplained and alarming increase in the incidence of colon cancer in people younger than 50," says Dr. Chan.
Overall, deaths from colon cancer dropped by 2% per year from 2011 to 2020. But that's not the case among people younger than 50. In that age group, deaths from colon cancer rose between 0.5% and 3% during the same time period, according to statistics published in 2023.
The rising rates of colon cancer in younger people are occurring in all racial and ethnic groups, with the steepest rises seen among Alaskan Natives and Native Americans. Overall, Blacks and African Americans are more likely to get and die from colon cancer than whites, and early-onset cases are higher in Black individuals than whites.
Efforts to encourage colon cancer screening began in the mid-1990s. Today, about 60% of adults over 50 follow the advice to receive a colonoscopy (described below) on a regular basis. This track record, while not perfect, likely explains the decline in deaths from colon cancer in older adults.
"I think that promoting earlier screening will help stem the rise in early-onset cases, at least for those in their 40s. We've also seen that earlier colonoscopies may be associated with lowering incidence of colon cancer even later in life, "says Dr. Chan.
What are the different screening tests for colon cancer?
The two most widely used screening tests are a standard colonoscopy and various stool-based tests.
Colonoscopy. For this test, a gastroenterologist or surgeon snakes a long, flexible tube with a camera on the end through your rectum and beyond to inspect the entire length of your colon. Considered the gold-standard test, this procedure can detect precancerous polyps called adenomas, and allow for their removal.
The test requires taking laxatives and drinking lots of fluids beforehand to clean all the fecal material (stool) out of your colon. Serious complications, which include perforation or bleeding, are rare, occurring in about three in 1,000 procedures. If no polyps are found, a repeat colonoscopy isn't recommended for another 10 years. If you have polyps, or your risk or symptoms change, this interval will be shorter.
Stool tests. The more worrisome colon polyps (adenomas) often shed tiny amounts of blood and abnormal DNA into the stool. This can be detected from samples you collect yourself at home.
- Two tests, the fecal occult blood test (FOBT) and fecal immunochemical test (FIT), check for blood. They require small stool samples that you put on a card or in a tube that's then mailed to a lab. These tests should be done every year.
- A third option, the FIT-DNA test, checks for both blood and abnormal DNA; it's usually repeated every three years.
Additionally, the guidelines from the American College of Physicians suggest another option: flexible sigmoidoscopy, which inspects only the lower part of the colon, once every 10 years, combined with a fecal FIT testing every two years. However, doctors in the United States rarely order sigmoidoscopy today.
If flexible sigmoidoscopy or any of these stool tests show evidence of a problem, a colonoscopy is needed to check for adenomas or cancer.
Why might stool-based screening make sense for younger adults?
Colonoscopy isn't necessarily the best initial screening test for everyone, says Dr. Chan. That's especially true for younger people, mainly because it's time-consuming and inconvenient.
"Maybe you just can't find time in your schedule or are worried about having a colonoscopy," he says. If that's the case, a stool-based test — which is noninvasive and takes very little time — is an appropriate option.
"The worst option is not doing anything, because early detection and treatment can prevent deaths," he says.
About the Author

Julie Corliss, Executive Editor, Harvard Heart Letter
Julie Corliss is the executive editor of the Harvard Heart Letter. Before working at Harvard, she was a medical writer and editor at HealthNews, a consumer newsletter affiliated with The New England Journal of Medicine. She … See Full Bio View all posts by Julie Corliss
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

Can AI answer medical questions better than your doctor?

Last year, headlines describing a study about artificial intelligence (AI) were eye-catching, to say the least:
- ChatGPT Rated as Better Than Real Doctors for Empathy, Advice
- The AI will see you now: ChatGPT provides higher quality answers and is more empathetic than a real doctor, study finds
- Is AI Better Than A Doctor? ChatGPT Outperforms Physicians In Compassion And Quality Of Advice
At first glance, the idea that a chatbot using AI might be able to generate good answers to patient questions isn’t surprising. After all, ChatGPT boasts that it passed a final exam for a Wharton MBA, wrote a book in a few hours, and composed original music.
But showing more empathy than your doctor? Ouch. Before assigning final honors on quality and empathy to either side, let’s take a second look.
What tasks is AI taking on in health care?
Already, a rapidly growing list of medical applications of AI includes drafting doctor’s notes, suggesting diagnoses, helping to read x-rays and MRI scans, and monitoring real-time health data such as heart rate or oxygen level.
But the idea that AI-generated answers might be more empathetic than actual physicians struck me as amazing — and sad. How could even the most advanced machine outperform a physician in demonstrating this important and particularly human virtue?
Can AI deliver good answers to patient questions?
It’s an intriguing question.
Imagine you’ve called your doctor’s office with a question about one of your medications. Later in the day, a clinician on your health team calls you back to discuss it.
Now, imagine a different scenario: you ask your question by email or text, and within minutes receive an answer generated by a computer using AI. How would the medical answers in these two situations compare in terms of quality? And how might they compare in terms of empathy?
To answer these questions, researchers collected 195 questions and answers from anonymous users of an online social media site that were posed to doctors who volunteer to answer. The questions were later submitted to ChatGPT and the chatbot’s answers were collected.
A panel of three physicians or nurses then rated both sets of answers for quality and empathy. Panelists were asked “which answer was better?” on a five-point scale. The rating options for quality were: very poor, poor, acceptable, good, or very good. The rating options for empathy were: not empathetic, slightly empathetic, moderately empathetic, empathetic, and very empathetic.
What did the study find?
The results weren’t even close. For nearly 80% of answers, ChatGPT was considered better than the physicians.
- Good or very good quality answers: ChatGPT received these ratings for 78% of responses, while physicians only did so on 22% of responses.
- Empathetic or very empathetic answers: ChatGPT scored 45% and physicians 4.6%.
Notably, the length of the answers was much shorter for physicians (average of 52 words) than for ChatGPT (average of 211 words).
Like I said, not even close. So, were all those breathless headlines appropriate after all?
Not so fast: Important limitations of this AI research
The study wasn’t designed to answer two key questions:
- Do AI responses offer accurate medical information and improve patient health while avoiding confusion or harm?
- Will patients accept the idea that questions they pose to their doctor might be answered by a bot?
And it had some serious limitations:
- Evaluating and comparing answers: The evaluators applied untested, subjective criteria for quality and empathy. Importantly, they did not assess actual accuracy of the answers. Nor were answers assessed for fabrication, a problem that has been noted with ChatGPT.
- The difference in length of answers: More detailed answers might seem to reflect patience or concern. So, higher ratings for empathy might be related more to the number of words than true empathy.
- Incomplete blinding: To minimize bias, the evaluators weren’t supposed to know whether an answer came from a physician or ChatGPT. This is a common research technique called “blinding.” But AI-generated communication does not always sound exactly like a human, and the AI answers were significantly longer. So, it’s likely that for at least some answers, the evaluators were not blinded.
The bottom line
Could physicians learn something about expressions of empathy from AI-generated answers? Possibly. Might AI work well as a collaborative tool, generating responses that a physician reviews and revises? Actually, some medical systems already use AI in this way.
But it seems premature to rely on AI answers to patient questions without solid proof of their accuracy and actual supervision by healthcare professionals. This study wasn’t designed to provide either.
And by the way, ChatGPT agrees: I asked it if it could answer medical questions better than a doctor. Its answer was no.
We’ll need more research to know when it’s time to set the AI genie free to answer patients’ questions. We may not be there yet — but we’re getting closer.
Want more information about the research? Read responses composed by doctors and a chatbot, such as answers to a concern about consequences after swallowing a toothpick.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD

Will miscarriage care remain available?

When you first learned the facts about pregnancy — from a parent, perhaps, or a friend — you probably didn’t learn that up to one in three ends in a miscarriage.
What causes miscarriage? How is it treated? And why is appropriate health care for miscarriage under scrutiny — and in some parts of the US, getting harder to find?
What is miscarriage?
Many people who come to us for care are excited and hopeful about building their families. It’s devastating when a hoped-for pregnancy ends early.
Miscarriage is a catch-all term for a pregnancy loss before 20 weeks, counting from the first day of the last menstrual period. Miscarriage happens in as many as one in three pregnancies, although the risk gradually decreases as pregnancy progresses. By 20 weeks, it occurs in fewer than one in 100 pregnancies.
What causes miscarriage?
Usually, there is no obvious or single cause for miscarriage. Some factors raise risk, such as:
- Pregnancy at older ages. Chromosome abnormalities are a common cause of pregnancy loss. As people age, this risk rises.
- Autoimmune disorders. While many pregnant people with autoimmune disorders like lupus or Sjogren’s syndrome have successful pregnancies, their risk for pregnancy loss is higher.
- Certain illnesses. Diabetes or thyroid disease, if poorly controlled, can raise risk.
- Certain conditions in the uterus. Uterine fibroids, polyps, or malformations may contribute to miscarriage.
- Previous miscarriages. Having a miscarriage slightly increases risk for miscarriage in the next pregnancy. For instance, if a pregnant person’s risk of miscarriage is one in 10, it may increase to 1.5 in 10 after their first miscarriage, and four in 10 after having three miscarriages.
- Certain medicines. A developing pregnancy may be harmed by certain medicines. It’s safest to plan pregnancy and receive pre-pregnancy counseling if you have a chronic illness or condition.
How is miscarriage diagnosed?
Before ultrasounds in early pregnancy became widely available, many miscarriages were diagnosed based on symptoms like bleeding and cramping. Now, people may be diagnosed with a miscarriage or early pregnancy loss on a routine ultrasound before they notice any symptoms.
How is miscarriage treated?
Being able to choose the next step in treatment may help emotionally. When there are no complications and the miscarriage occurs during the first trimester (up to 13 weeks of pregnancy), the options are:
Take no action. Passing blood and pregnancy tissue often occurs at home naturally, without need for medications or a procedure. Within a week, 25% to 50% will pass pregnancy tissue; more than 80% of those who experience bleeding as a sign of miscarriage will pass the pregnancy tissue within two weeks.
What to know: This can be a safe option for some people, but not all. For example, heavy bleeding would not be safe for a person who has anemia (lower than normal red blood cell counts).
Take medication. The most effective option uses two medicines: mifepristone is taken first, followed by misoprostol. Using only misoprostol is a less effective option. The two-step combination is 90% successful in helping the body pass pregnancy tissue; taking misoprostol alone is 70% to 80% successful in doing so.
What to know: Bleeding and cramping typically start a few hours after taking misoprostol. If bleeding does not start, or there is pregnancy tissue still left in the uterus, a surgical procedure may be necessary: this happens in about one in 10 people using both medicines and one in four people who use only misoprostol.
Use a procedure. During dilation and curettage (D&C), the cervix is dilated (widened) so that instruments can be inserted into the uterus to remove the pregnancy tissue. This procedure is nearly 99% successful.
What to know: If someone is having life-threatening bleeding or has signs of infection, this is the safest option. This procedure is typically done in an operating room or surgery center. In some instances, it is offered in a doctor’s office.
If you have a miscarriage during the second trimester of pregnancy (after 13 weeks), discuss the safest and best plan with your doctor. Generally, second trimester miscarriages will require a procedure and cannot be managed at home.
Red flags: When to ask for help during a miscarriage
During the first 13 weeks of pregnancy: Contact your health care provider or go to the emergency department immediately if you experience
- heavy bleeding combined with dizziness, lightheadedness, or feeling faint
- fever above 100.4° F
- severe abdominal pain not relieved by over-the-counter pain medicine, such as acetaminophen (Tylenol) or ibuprofen (Motrin, Advil). Please note: ibuprofen is not recommended during pregnancy, but is safe to take if a miscarriage has been diagnosed.
After 13 weeks of pregnancy: Contact your health care provider or go to the emergency department immediately if you experience
- any symptoms listed above
- leakage of fluid (possibly your water may have broken)
- severe abdominal or back pain (similar to contractions).
How is care for miscarriages changing?
Unfortunately, political interference has had significant impact on safe, effective miscarriage care:
- Some states have banned a procedure used to treat second trimester miscarriage. Called dilation and evacuation (D&E), this removes pregnancy tissue through the cervix without making any incisions. A D&E can be lifesaving in instances when heavy bleeding or infection is complicating a miscarriage.
- Federal and state lawsuits, or laws banning or seeking to ban mifepristone for abortion care, directly limit access to a safe, effective drug approved for miscarriage care. This could affect miscarriage care nationwide.
- Many laws and lawsuits that interfere with miscarriage care offer an exception to save the life of a pregnant patient. However, miscarriage complications may develop unexpectedly and worsen quickly, making it hard to ensure that people will receive prompt care in life-threatening situations.
- States that ban or restrict abortion are less likely to have doctors trained to perform a full range of miscarriage care procedures. What’s more, clinicians in training, such as resident physicians and medical students, may never learn how to perform a potentially lifesaving procedure.
Ultimately, legislation or court rulings that ban or restrict abortion care will decrease the ability of doctors and nurses to provide the highest quality miscarriage care. We can help by asking our lawmakers not to pass laws that prevent people from being able to get reproductive health care, such as restricting medications and procedures for abortion and miscarriage care.
About the Authors

Sara Neill, MD, MPH, Contributor
Dr. Sara Neill is a physician-researcher in the department of obstetrics & gynecology at Beth Israel Deaconess Medical Center and Harvard Medical School. She completed a fellowship in complex family planning at Brigham and Women's Hospital, and … See Full Bio View all posts by Sara Neill, MD, MPH 
Scott Shainker, DO, MS, Contributor
Scott Shainker, D.O, M.S., is a maternal-fetal medicine specialist in the Department of Obstetrics and Gynecology at Beth Israel Deaconess Medical Center (BIDMC). He is also a member of the faculty in the Department of Obstetrics, … See Full Bio View all posts by Scott Shainker, DO, MS
Ready to give up the lead vest?

At a dental appointment last month, I spotted a lead vest hanging unassumingly on the wall of the exam room as soon as I walked in. “Still there, but now obsolete,” I thought.
I’d just learned about new guidelines from the American Dental Association (ADA) saying lead vests and thyroid collars that cover the neck are no longer needed during dental x-rays. But they’d been a fixture of my dental experiences — including many cavities, four root canals, a tooth extraction, and two crowns — for my entire life. What changed, and could I feel safe without the vest?
Why were lead vests used in past years?
Lead vests and thyroid collars have been worn by countless Americans during dental x-rays over the years. They’ve been in use for far longer than my lifetime — about 100 years. The heavy apron-like shields are placed over sensitive areas, including the chest and neck, before the x-rays are taken.
“I haven’t worn a lead apron in the last 10 or 15 years — unless a dentist insists I put it on — because I know it isn’t needed,” says Dr. Bernard Friedland, an associate professor of oral medicine, infection, and immunity at Harvard School of Dental Medicine.
What has changed about dental x-rays?
When lead vests and thyroid collars were first recommended, x-ray technology was much less precise. But the technology has evolved significantly over the last few decades in ways that dramatically improve patient safety:
- Digital x-rays enable far smaller radiation doses, reducing radiation exposure and the risks associated with higher doses, such as cancer. “The doses used in dental radiology are negligibly small now. If you go to the dentist today for a full series of mouth x-rays that are taken with a digital sensor, the total exposure time is just over five seconds,” explains Dr. Friedland, an expert in oral radiology. “A hundred or so years ago, that exposure time would have been many minutes.”
- The small size of today’s x-ray beam significantly reduces radiation “scatter” and restricts the beam size to only the area needing to be imaged. This protects patients from radiation exposure to other parts of the body.
A less-recognized strike against using lead vests and thyroid collars is their ability to get in the way. They may block the primary x-ray beam, preventing dentists from capturing needed images. This quirk can lead to repeat imaging and unnecessary exposure to additional radiation. This is more likely to occur with panoramic x-rays.
The gear may also spread germs, Dr. Friedland notes. Although disinfected, it’s not sterilized between uses. “There’s a risk of spreading bacteria and viruses,” he says. “To me, that’s also an issue and another reason I don’t want to use one on myself.”
Who no longer needs the shields?
No one does — even children, who presumably have a long life of dental x-rays in front of them. The new recommendations apply to all patients regardless of age, health status, or pregnancy, the ADA says.
The recommendation to discontinue lead vests has been a long time in the making. In fact, the ADA isn’t the first professional organization to propose it. The American Association of Physicists in Medicine did so in 2019, followed by the American College of Radiology in 2021 and the American Academy of Oral and Maxillofacial Radiology in 2023.
Are some people confused or concerned about the no-lead-vest policy?
Yes. The new guidelines are bound to draw confusion and fear, Dr. Friedland says. Some people may even insist on continuing to wear a lead vest during x-rays.
“A big problem is that people’s perception of risk is very skewed,” he says. “Some people, you’ll never convince.”
People are likely to feel more comfortable if the practice is uniformly adopted by dentists. However, the ability to implement this change may hinge partly on public response. And it could take a while to fully adopt.
“I think the public is going to have more say on this than dentists,” Dr. Friedland says. “It might take a generation to make this change, maybe longer.”
Still concerned about the new recommendations?
If you have lingering concerns about the new recommendations, talk to your dentist.
And ask if dental x-rays are necessary to proceed with your diagnosis or treatment plan. Sometimes it’s possible to take fewer x-rays — such as bitewing x-rays of the upper and lower back teeth only — or to use certain types of imaging less frequently. Even with far safer x-ray conditions, dentists should be able to justify that the information from images is integral to diagnose problems or improve care, Dr. Friedland says.
It’s worth noting that the dose of radiation, while far lower than in the past, varies with the type of imaging and which parts of the jaw are being imaged. For example, the digital dental x-rays mentioned above involve less radiation than conventional dental x-rays. Either panoramic dental x-rays, or 3-D dental x-rays taken with a CBCT system that rotates around the head, typically involve more radiation than conventional dental x-rays.
Whenever possible, dentists should use images taken during previous dental exams, according to the ADA. “If I don’t need an x-ray, I don’t get one,” says Dr. Friedland. “I’m not cavalier about it. I also use technical parameters that keep the x-ray dose as low as reasonably possible.”
About the Author

Maureen Salamon, Executive Editor, Harvard Women's Health Watch
Maureen Salamon is executive editor of Harvard Women’s Health Watch. She began her career as a newspaper reporter and later covered health and medicine for a wide variety of websites, magazines, and hospitals. Her work has … See Full Bio View all posts by Maureen Salamon
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD
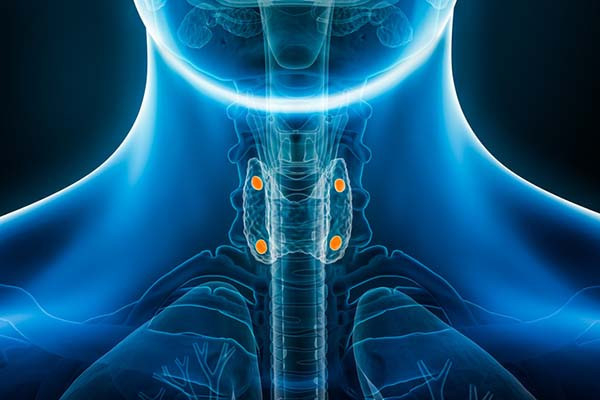
Your amazing parathyroid glands

You probably know that you have a thyroid gland. Perhaps you or someone you know has had thyroid tests or a thyroid disorder such as hypothyroidism.
But did you know you also have a parathyroid gland? It’s true — in fact, most people have four of them, even though one would suffice.
Where are the parathyroid glands?
From the name, you might assume the role of the parathyroid glands is related to that of the thyroid gland. Well, you’d be wrong. The name comes solely from their location: they sit just behind the thyroid gland: two on the right side, two on the left.
The parathyroid glands are small (the size of peas), and can weigh less than a thousandth of an ounce each. Although it’s normal to have four parathyroid glands, about 13% of people have fewer and 5% have more. And some people have parathyroid glands in other locations, such as alongside the esophagus or in the chest. This variation rarely matters, unless surgery is necessary to remove one or more of them.
What do the parathyroid glands do?
Logically enough, parathyroid glands make parathyroid hormone (PTH). And what does PTH do? It has several functions, including:
- Regulating calcium: Calcium is a mineral with many essential roles throughout the body, such as maintaining bone strength, allowing nerves and muscles to function normally, and making sure blood clots as it should. Higher levels of PTH lead to higher calcium levels in the blood through actions on the kidneys and bones.
- Regulating phosphorus: Among other roles, this mineral is a key component of our DNA, bones, and teeth. Phosphorus activates essential enzymes throughout the body, including enzymes necessary for cell reproduction and survival. It also helps with nerve and muscle function.
- Regulating vitamin D: This vitamin is actually a hormone that helps maintain normal levels of calcium throughout the body, by controlling how much gets absorbed from food in the intestinal tract and how much is lost by the kidneys in your urine. Remember PTH? Well, PTH regulates production of the enzyme that converts inactive vitamin D to an active form that helps your gut absorb calcium and reduces the loss of calcium in urine.
PTH released by the parathyroid glands helps keep each of these nutrients in balance. For example, if your blood calcium level falls, your parathyroid glands make more PTH. Higher amounts of PTH prompt bones to release stored calcium into the bloodstream, and also signal the kidneys to pull back on the amount of calcium lost through urine.
What if your blood calcium level rises? Then the parathyroid glands make less PTH, which helps to correct the blood calcium level.
Which diseases involve the parathyroid glands?
The most common are:
- Hyperparathyroidism: This is a condition in which the parathyroid glands make more than the normal amount of PTH. This can be due to a benign or cancerous tumor on a single gland, or due to multiple glands becoming overactive. Or it may be due to some other trigger, such as a low level of calcium in the blood, inadequate vitamin D levels, or kidney failure. When there’s too much PTH, blood calcium levels can become dangerously high and phosphorus levels fall. Surgery may be recommended to remove the overactive gland or glands.
- Hypoparathyroidism: This rare condition is diagnosed when less than the normal amount of PTH is produced. The most common causes are prior neck surgery or radiation, autoimmune disease, or low magnesium levels.
- Parathyroid cancer: Risk factors for parathyroid cancer include certain genetic diseases and prior radiation to the neck.
Why do we rarely hear about the parathyroid glands?
The reason is that most of the time they do their job without fuss or fanfare. Although disorders of the parathyroid glands are not rare, they are just uncommon enough that most people will never hear about them. I think of the parathyroid glands as one of many parts of our bodies that play a huge role in our health, but go unappreciated because they are so good at what they do.
Many other quiet heroes, including the thymus gland, serve as testaments to the remarkable design and function of the human body. Then again, I can think of a few body parts that could be considered expendable.
The bottom line
I hope it’s comforting to know that your amazing parathyroid glands are keeping tabs on your calcium levels and helping your bones, nerves, muscles, and other organs to function normally.
Ounce for ounce, the parathyroid glands may be the most important glands you’d never heard of. Until now.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD

Dog bites: How to prevent or treat them
 Each year, more than 4.5 million dog bites occur in the United States. Despite what you might assume, most of these incidents don’t happen when an unfamiliar dog attacks someone in a park or another outdoor location. Instead, most dog bites are inflicted by a pet dog in a home.
Each year, more than 4.5 million dog bites occur in the United States. Despite what you might assume, most of these incidents don’t happen when an unfamiliar dog attacks someone in a park or another outdoor location. Instead, most dog bites are inflicted by a pet dog in a home.
Here’s advice for avoiding these upsetting and potentially serious injuries — and the steps you should take if you sustain a dog bite.
Why do dog bites happen?
Some dog bites happen by accident when people wrestle or play tug-of-war with their dog. But most of the time, dogs bite people as a reaction to feeling stressed, threatened, scared, or startled, according to the American Veterinary Medical Association (AVMA). More than half of dog bites occur in children, and they’re far more likely to be seriously injured than adults.
“People don’t always heed the behavioral signals that a dog is uncomfortable,” says Dr. Christopher Baugh, associate professor of emergency medicine at Harvard Medical School. For example, some dogs are highly territorial and will bark, growl, snap, and lunge if outsiders enter their space — whether that’s an apartment, yard, or crate. Or dogs may exhibit resource guarding, which shows up as anxious, aggressive behavior around food, toys, or beds.
“These situations can be high-risk, and children in particular have less awareness of that risk,” says Dr. Baugh, who has children and two mixed-breed rescue dogs, Harley and Roxi.
What can you do to prevent dog bites?
Any dog — even a sweet, cuddly dog — can bite if provoked, according to the AVMA. Never leave young children alone with a dog without adult supervision. And teach children to never disturb a dog while it’s eating, sleeping, or caring for puppies.
In a study of 321 facial dog bites treated at Harvard-affiliated Massachusetts General Hospital over a 20-year period, 88% of the bites were from known dogs. Most were in adults and occurred after playing with the dog, feeding the dog, and placing their face close to the dog. However, the hand (usually a person’s dominant hand) is probably the most common location for a dog bite in an adult, says Dr. Baugh.
Other tips from the CDC to prevent dog bites include the following:
- Always ask a dog’s owner if it’s okay to pet their dog, even if the dog appears friendly.
- Make sure the dog sees and sniffs you before reaching out to pet it.
- Don’t pet a dog that seems to be hiding, scared, sick, or angry.
What if an unfamiliar dog approaches you? Remain calm and still, avoiding eye contact with the dog. Stand with the side of your body facing the dog and say “no” or “go home” in firm, deep voice. Wait for the dog to retreat or move yourself slowly away.
What should you do if you’re bitten by a dog?
Clean the wound with mild soap and running water, then cover it with a clean bandage or cloth. Some online resources recommend applying an antibiotic ointment or cream. But these products are recommended only for people with clear evidence of an infection, such as redness, pus, pain, swelling, or warmth, according to the American Academy of Dermatology.
If the injury is serious — with a bite on the face, heavy bleeding, or a possible broken bone — go to the emergency room. That’s also a good idea if you’re bitten by an unknown or stray dog, in the rare event that you might need medicines to prevent rabies (rabies post-exposure prophylaxis).
“Often, people are shocked after being bit and will understandably focus all their attention on their wound,” says Dr. Baugh. The dog’s owner may check in to see if you’re okay, but then walk away. But you should get the person’s contact information and make sure the dog is vaccinated against rabies, he says.
Keep in mind that:
- Emergency rooms are often crowded with long waits, so an urgent care clinic is a good option if the injury doesn’t require immediate attention.
- Some wounds require stitches, ideally within 12 to 24 hours.
- The doctor may prescribe antibiotics to prevent possible infections, especially if you have health problems such as a weakened immune system or diabetes.
- You may also need a tetanus booster if you haven’t had one in the past 10 years. If your vaccine history isn’t available or you can’t remember, you’ll get a tetanus booster just in case.
What if a dog bite is less serious?
Let’s say you have a less serious bite from a family dog known to have a current rabies vaccine. Bites that don’t require stitches can be cleaned with mild soap and running water, then evaluated by your regular health care provider. They may tell you to simply monitor the wound for signs of infection.
“Doctors are trying to be more thoughtful about prescribing antibiotics and limit their use in low-risk situations, because overuse contributes to antibiotic resistance and exposes people to potential side effects without any benefit,” says Dr. Baugh.
About the Author

Julie Corliss, Executive Editor, Harvard Heart Letter
Julie Corliss is the executive editor of the Harvard Heart Letter. Before working at Harvard, she was a medical writer and editor at HealthNews, a consumer newsletter affiliated with The New England Journal of Medicine. She … See Full Bio View all posts by Julie Corliss
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

How well do you worry about your health?

Don’t worry. It’s good advice if you can take it. Of course that’s not always easy, especially for health concerns.
The truth is: it’s impossible (and ill-advised) to never worry about your health. But are you worrying about the right things? Let’s compare a sampling of common worries to the most common conditions that actually shorten lives. Then we can think about preventing the biggest health threats.
Dangerous but rare health threats
The comedian John Mulaney says the cartoons he watched as a child gave him the impression that quicksand, anvils falling from the sky, and lit sticks of dynamite represented major health risks. For him (as is true for most of us), none of these turned out to be worth worrying about.
While harm can befall us in many ways, some of our worries are not very likely to occur:
- Harm by lightning: In the US, lightning strikes kill about 25 people each year. Annually, the risk for the average person less than one in a million. There are also several hundred injuries due to nonfatal lightning strikes. Even though lightning strikes the earth millions of times each year, the chances you’ll be struck are quite low.
- Dying in a plane crash: The yearly risk of being killed in a plane crash for the average American is about one in 11 million. Of course, the risk is even lower if you never fly, and higher if you regularly fly on small planes in bad weather with inexperienced pilots. By comparison, the average yearly risk of dying in a car accident is approximately 1 in 5,000.
- Snakebite injuries and deaths: According to the Centers for Disease Control and Prevention, an estimated 7,000 to 8,000 people are bit by poisonous snakes each year in the US. Lasting injuries are uncommon, and deaths are quite rare (about five per year). In parts of the country where no poisonous snakes live, the risk is essentially zero.
- Shark attacks: As long as people aren’t initiating contact with sharks, attacks are fairly uncommon. Worldwide, about 70 unprovoked shark attacks occur in an average year, six of which are fatal. In 2022, 41 attacks occurred in the US, two of which were fatal.
- Public toilet seats: They may appear unclean (or even filthy), but they pose little or no health risk to the average person. While it’s reasonable to clean off the seat and line it with paper before touching down, health fears should not discourage you from using a public toilet.
I’m not suggesting that these pose no danger, especially if you’re in situations of increased risk. If you’re on a beach where sharks have been sighted and seals are nearby, it’s best not to swim there. When in doubt, it’s a good idea to apply common sense and err on the side of safety.
What do Google and TikTok tell us about health concerns?
Analyzing online search topics can tell us a lot about our health worries.
The top Google health searches in 2023 were:
- How long is strep throat contagious?
- How contagious is strep throat?
- How to lower cholesterol?
- What helps with bloating?
- What causes low blood pressure?
Really? Cancer, heart disease and stroke, or COVID didn’t reach the top five? High blood pressure didn’t make the list, but low blood pressure did?
Meanwhile, on TikTok the most common topics searched were exercise, diet, and sexual health, according to one study. Again, no top-of-the-list searches on the most common and deadly diseases.
How do our worries compare with the top causes of death?
In the US, these five conditions took the greatest number of lives in 2022:
- heart disease
- cancer
- unintentional injury (including motor vehicle accidents, drug overdoses, and falls)
- COVID-19
- stroke.
This list varies by age. For example, guns are the leading cause of death among children and teenagers (ages 1 to 19). For older teens (ages 15 to 19), the top three causes of death were accidents, homicide, and suicide.
Perhaps the lack of overlap between leading causes of death and most common online health-related searches isn’t surprising. Younger folks drive more searches and may not have heart disease, cancer, or stroke at top of mind. In addition, online searches might reflect day-to-day concerns (how soon can my child return to school after having strep throat?) rather than long-term conditions, such as heart disease or cancer. And death may not be the most immediate health outcome of interest.
But the disconnect suggests to me that we may be worrying about the wrong things — and focusing too little on the biggest health threats.
Transforming worry into action
Most of us can safely worry less about catching something from a toilet seat or shark attacks. Instead, take steps to reduce the risks you face from our biggest health threats. Chipping away at these five goals could help you live longer and better while easing unnecessary worry:
- Choose a heart-healthy diet.
- Get routinely recommended health care, including blood pressure checks and cancer screens, such as screening for colorectal cancer.
- Drive more safely. Obey the speed limit, drive defensively, always wear a seatbelt, and don’t drive if you’ve been drinking.
- Don’t smoke. If you need to quit, find help.
- Get regular exercise.
The bottom line
Try not to focus too much on health risks that are unlikely to affect you. Instead, think about common causes of poor health. Then take measures to reduce your risk. Moving more and adding healthy foods to your meals is a great start.
And in case you’re curious, the average number of annual deaths due to quicksand is zero in the US. Still a bit worried? Fine, here’s a video that shows you how to save yourself from quicksand even though you’ll almost certainly never need it.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD